Patient Education
Learn more about eye health, our diagnostic procedures, and the advanced surgical treatments we offer.
See Right
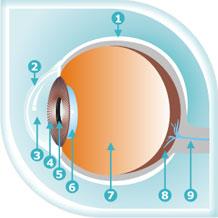
The mechanism that makes the eye
Your eyes are at work from the moment you wake up, to the time you close them and go to sleep. They assimilate information about the world around you. Eyes perceive shapes, sense colors and distinguish movements. Little do we realise that all these functions that our eyes perform, are stitched together by a complex mechanism that works in coordination with our brain to complete the process of visual perception and processing.
Let us briefly look at the various components that make up our eyes:
The white part of the eyeball is called the sclera. The sclera is made up of a tough material and covers most of the eyeball. It also has visible red blood vessels that deliver blood to it.
The cornea is a transparent protruding dome in front of the coloured part of the eye. The cornea helps the eye focus as light makes its way through.
Immediately behind the cornea is the anterior chamber, a space filled with a transparent fluid that nourishes the eye and keeps it healthy.
After the anterior chamber is the iris that lends the eye its natural colour. The iris has muscles attached to it that changes its shape, and thus regulates the entry of light.
The pupil is the black circlular opening in the center of the iris, that allows and controls the amount of light that enters. The pupils become small when the light is bright and opens wider when the light is less.
After the light enters the pupil, it hits the lens. The lens is behind the iris and is clear and colourless. The lens' job is to focus the light rays to the back of the eyeball.
The light from the lens passes through the vitreous body which is the biggest part of the eye, forms two thirds of the eye's volume and gives the eye its shape. It is filled with a clear, jelly like material called the vitreous humour. After the light passes through the lens, it shines straight through the vitreous humour to the back of the eyeball.
At the very back of the eyeball is the retina which holds millions of cells called rods and cones to process light. Rods see in black, white and shades of gray and allow us to see even when it's very dark. Cones sense colour and require light to function properly. Cones are of three types each sensitive to shades of either red, green or blue. Together, these cones can sense combinations of light waves that enable our eyes to see millions of colours.
The colours and image sensed by the retina is then informed to the brain with the help of nerves called the optic nerves. The brain then logically identifies what the eye sees, thereby helping our minds to relate to it.
Now that we know the mechanism, let’s look at a few tips for eye care.
Simple tips for healthy eyes
Staying healthy is a personal choice. And one has to work really hard for it. A balanced diet, good amount of sleep, balance between work and rest, and exercise - all play a vital role in restoring our health and helping us maintain our eyesight. However, here we’ve shared simple day-to-day do's and don'ts which will help you maintain a healthy eyesight.
While working on a computer:
- Ensure the monitor is 6-8 inches below the eye level
- Maintain a distance of 20-30 inches between your seat and the screen
- Use anti-reflective coating on the monitor
- Wear anti-glare glasses
- Blink frequently to prevent dehydration
- Give your eyes frequent breaks while working for prolonged hours
- Avoid sitting opposite to an AC vent as it can dry up your eyes
- Take a stroll outside to get your eyes some fresh air
While using contact lenses:
- To prevent infections avoid wearing contact lenses for more than 10-12 hours a day
- While swimming never wear contact lenses. The microorganisms and chlorine in the water can cause infections and/or damage your contact lenses
While driving:
- While driving at night, use anti-glare glasses to protect your eyes from the focus of headlights
- While driving during the day, wear UV-protective glasses
- Choose glasses that cover the sides of your eyes as well
While planning daily meals:
- Ensure intake of citrus fruits, green leafy vegetables, tomatoes, spinach, poultry and dairy products
- Pack a box of chopped carrots, cucumber and fresh fruits and munch in-between meals at the office
To reduce puffiness around the eyes:
- Refrigerate used tea bags and later place them on your eyes
- Drink plenty of water and keep yourself hydrated. When a person is dehydrated, especially in an air-conditioned office, the body starts storing water as a defence mechanism. This causes puffiness
If dirt enters your eyes:
- Avoid rubbing as this may cause the dirt to stick inside
- Blink several times to start your tears flowing and flush out the dirt
In case of alcohol and smoking addictions:
- Reduce the smoking and alcohol intake. Both nicotine and alcohol are nerve toxins, they weaken the optic nerves in the long run
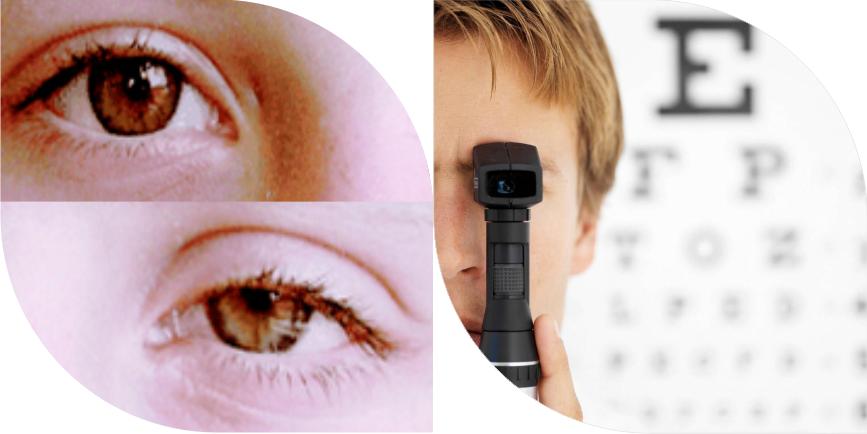
While getting your eyes tested:
- Visit an eye doctor (ophthalmologist) and not an optician. Remember, a doctor can detect even hidden symptoms of eye diseases, while an optician can only read the power of your eyes
Read more about the eye diseases - risk groups.
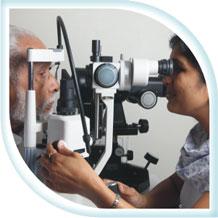
Thorough examination for thorough clarity
Irrespective of your age or physical health, it is important for everyone to have regular eye exams.
When an eye specialist examines your eyes, he or she also checks whether you need glasses.
How is this different from getting eyes checked at an optical outlet?
There is a difference between getting your number checked at an optical outlet versus undergoing an eye examination by an ophthalmologist. Your ophthalmologist conducts a comprehensive eye checkup for hidden abnormalities which is not so in the earlier case.
What constitutes a comprehensive eye examination?
You will be asked about your general health, medications you may be taking, your working environment, hobbies, etc. You will also be asked about any vision problems you may have been experiencing.
Using a visual acuity chart and a reading card, your eye specialist will assess your ability to see small details clearly at both near and far distances. Any refractive errors will be detected and corrective measures will be suggested using a combination of lenses. Your eye specialist will systematically change the lens combination until a clear focus is obtained.
Using a number of tests, your eye doctor will evaluate how well your eyes align or coordinate when working together and individually.
The front portion of the eye is examined in detail using a special instrument called slit lamp.
It is a process to measure the pressure in the eye and is an important test in detecting glaucoma.
You will be administered dilating drops to see the back portion of the eye (retina) using the indirect ophthalmoscope.
Other tests may be undertaken to evaluate your ability to change focus, see colour correctly, or perceive depth correctly.
Any patient who walks in at Shree Eye Care with any kind of problem has to undergo a comprehensive eye checkup to help the doctor understand the patient’s total eye anatomy and history and solve the case with more clarity and confidence. We are equipped with the latest technologies for an accurate and comprehensive eye checkup to ensure the best for you.

Be alert and cut down on risks
How often do you visit an eye doctor? Not until the need arises, right? Many a times, eye problems are triggered by external factors. Such problems are revealed through notable symptoms, and they prompt us to avail the expertise of an eye doctor immediately.
However, this is just half the truth.
There is another category of eye problems that are a direct result of a long-term build-up of internal complications. These are silent killers of eyesight and do not exhibit marked symptoms, until they get escalated to an advanced stage. By the time such problems are diagnosed, they would have reached a level wherein only complex treatment procedures would work. In some cases, the eye problems could also be deemed ‘incurable’. However, awareness about such disorders and undertaking requisite precautionary checkups can help us stay clear of their advents.
In this section we detail certain risk groups, which are more likely to contract such silent yet grave eye disorders:
Which are the risk groups?
Adults: Adults over 40 should have their eyes tested to check if their current prescriptions need any overhauling and to check for early signs of eye disease or sight deterioration.
Children: Vision is closely linked to the learning process. Many a times, children will not complain of vision problems simply because they don't know what ‘normal’ vision looks like. If your child performs poorly at school,
or exhibits a reading or learning disability, be sure to have his or her eyes examined to rule out an underlying visual cause.
Diabetics: Diabetics should undergo a comprehensive eye checkup once in 6 months, or as advised by your ophthalmologist. To read more on the connection of eye diseases with diabetes, click here.
See Better
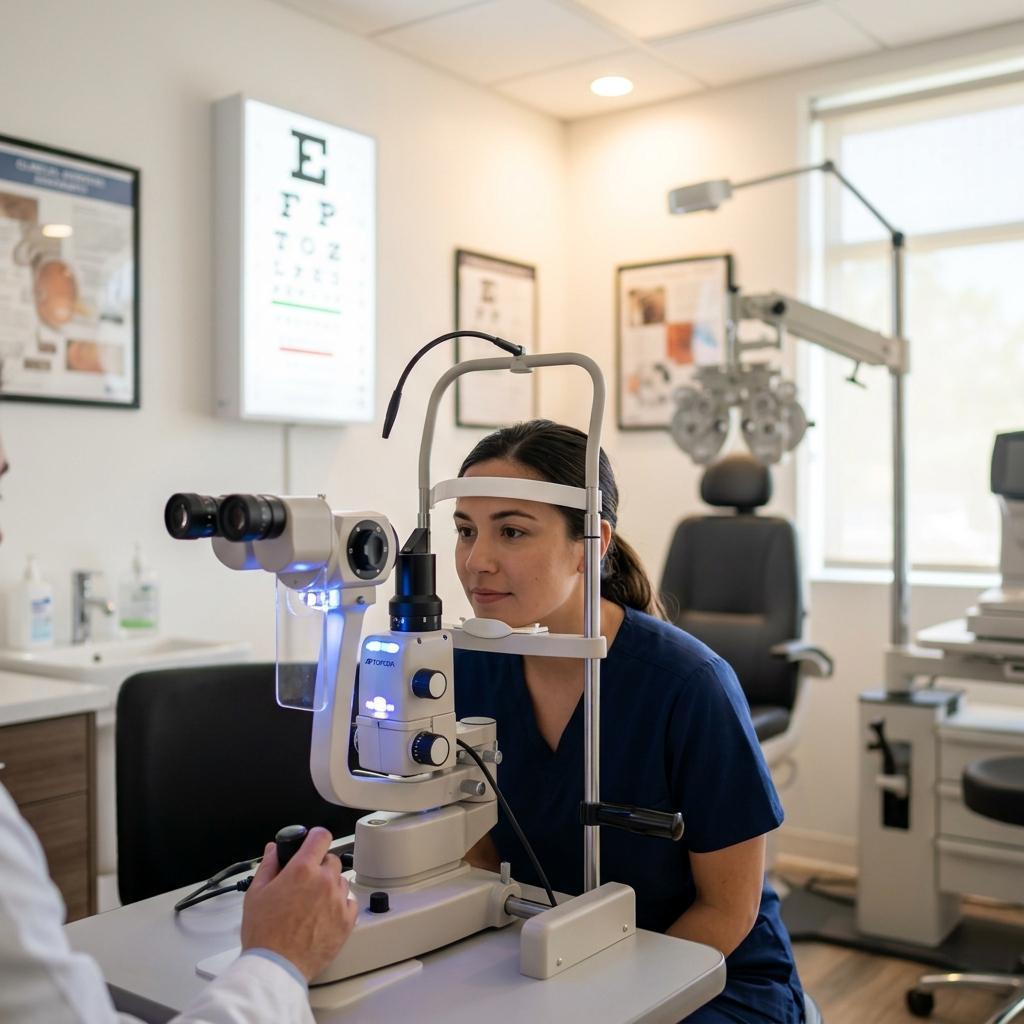

What is refractive disorder?
Refractive disorder is a commonly found structural disorder of the eye that makes it difficult for the eyes to sharply focus the light rays on the retina, thus resulting in a blurry vision. There are 3 types of refractive disorders.
Nearsightedness: In nearsightedness, closeby objects can be seen clearly but, those beyond a particular distance appear blurry. It is caused either by a change in the cornea or the lens or by a natural change in the shape of the eyeball.
Farsightedness: In farsightedness, objects at a distance appear clear whereas closeby objects appear blurry. Farsightedness is caused when your eye is too short lengthwise causing an image to focus behind the retina instead of directly on it.
Astigmatism: In astigmatism, objects at any distance appear blurry and wavy. The eye of a person with astigmatism is shaped like the back of a spoon. Hence, when light enters the eye, it is not refracted equally, allowing only a part of the object to be in focus.
Read more on refractive disorders in Treatments & Surgeries sections.
What is Computer Vision Syndrome (CVS)?
CVS is a temporary discomfort resulting from focusing the eyes on a computer screen for prolonged and uninterrupted periods of time.
What are the symptoms of CVS?
- Headaches
- Eye strain
- Blurred vision
- Dry, irritated eyes
- Neck pain
- Fatigue
- Difficulty in refocusing
- Double vision
What are the causes of CVS?
- Poor lighting
- Glare on the computer screen
- Poor seating posture
- Untreated vision problems
- Incorrect viewing distances
- Infrequent blinking. Usually, we blink around 22 times a minute. But, while looking at the computer screen, we hardly blink around 7 times
To read more on the treatment options available for CVS, visit the Treatments section.
What is cataract?
Cataract is the clouding of lens of the eye that leads to blurred vision.
What are the symptoms of cataract?
- Blurred vision
- Dulled colour vision
- Difficulty with glare
- Double vision
- Frequent changes in number
If not treated promptly, cataracts can also lead to blindness.
Am I at risk?
Yes you are, if you have any of the following risk factors:
- Aging, diabetes and long-term usage of drugs
- Eye impairments and perforations
- Long-term exposure to UV light without protection
To know further on cataract read Treatments & Surgeries sections.
How can diabetes affect the eye?
Diabetes can affect the eyes and vision in a number of ways. It may lead to:
- Frequent fluctuations in vision
- Cataract at a young age
- Decreased vision due to involvement of optic nerve
- Temporary paralysis of the muscles controlling the movement of eyes, thus leading to double vision
- Increased chances of contracting glaucoma
Beyond these ailments, the most significant complication of diabetes in the eye is diabetic retinopathy.
What is diabetic retinopathy?
Diabetes affects the small vessels of the retina in the eye. There are various stages of diabetic retinopathy:
Non-proliferative or background diabetic retinopathy: This is an early form of diabetic retinopathy and may not lead to any decrease in vision, but can lead to other more serious forms of retinopathy that affect the vision.
Diabetic maculopathy: Vision is usually not affected until macula, a part of the eye is involved. Macula if involved, the patient experiences gradual, progressive reduction in vision, for both distant and near objects.
Proliferative diabetic retinopathy: This is an advanced stage of diabetic retinopathy, where the blood supply of the retina reduces substantially. In response to this, new fragile blood vessels grow on the surface of the retina. These new vessels are very fragile and bleed easily. These may lead to serious vision problems like vision loss and blurred vision.
The longer a person has had diabetes, greater are his/her chances of contracting diabetic retinopathy. Almost 80% of people who have had diabetes for 15 years or more, suffer from retinal problems.
Can diabetic retinopathy spur other eye disorders as well?
The process also causes scar tissues to develop, which can pull the retina away from the back of the eye. This is known as retinal detachment, and can lead to blindness if untreated.
In addition, abnormal blood vessels can grow on the iris (the coloured part in the front of your eye) which can lead to glaucoma.
Can something be done to prevent diabetic retinopathy?
There is no treatment as such to prevent diabetic retinopathy altogether. Besides a good control of blood sugar, one must exercise regularly, keep blood pressure under control, avoid smoking and avoid obesity.
How do I know if I have diabetic retinopathy?
You might not know that you are having diabetic retinopathy, as there are no symptoms in the earlier stages of the disease. Therefore it is essential to have periodic evaluation of your eye by an ophthalmologist to detect the condition early. Early diagnosis and timely treatment is very essential in preventing the complications of this disease and thus maintaining clear vision.
If I have diabetes, how frequently should I get my eye examined?
If you have diabetes, you should get a yearly examination with your ophthalmologist. Once you are diagnosed with diabetic retinopathy, the frequency of visits will vary in accordance with the severity of the disease.
What are the common tests done for diabetic retinopathy?
First your vision is tested with the alphabet chart.
The back of your eye is then examined after dilating your pupils, using an instrument called ophthalmoscope.
Sometimes your ophthalmologist may advise a special test called fluorescein angiography, which is a test in which a series of photographs of the retina are taken with the help of a special camera. These photographs are taken after giving the patient an injection of a yellow dye. This dye reaches the retina through the blood stream and helps in seeing the blood vessels of retina more clearly. This test helps the doctor to determine further course of treatment.
What is Dry Eye Syndrome?
Dry Eye Syndrome is a disease where the eye loses the ability of keeping itself sufficiently lubricated either due to decreased tear production or increased tear film evaporation.
How do I know if I have dry eyes?
Frequent irritation, burning sensation, itching, foggy vision, sensing the presence of some foreign particle in the eye, eye pain and fatigue are some of the common symptoms of dry eye syndrome.
What are the causes of dry eye syndrome?
Aging, hormonal changes, autoimmune diseases and some medications can result in poor production of tears. People who sit in front of the PC for long hours are also susceptible to dry eye syndrome.
Evaporative loss of the watery tear layer is usually a result of an insufficient overlying lipid layer.
Your cornea specialist would conduct a battery of dry eye tests to determine the cause of your dry eye. In some cases, a blood checkup for autoimmune diseases may also be suggested.
What if dry eye is not treated in time?
Dry eye syndrome if not diagnosed and treated in time, can lead to patient resorting to remedies like rose water, netraprabha, honey and so on. Using such products can be counterproductive.
Prolonged dry eye can reduce work efficiency. Severe dry eye can also lead to corneal infections and perforations.
To know further on the treatment options available for dry eye syndrome, refer to the Treatments section.
How does the cornea get diseased?
- Corneal opacity
- Infections
- Diseased cornea at birth
- Injuries
- Malnutrition
- Chemical burns
- Congenital disorders
To know more about the treatment options available for corneal diseases, refer to corneal transplantation in the Surgeries section.
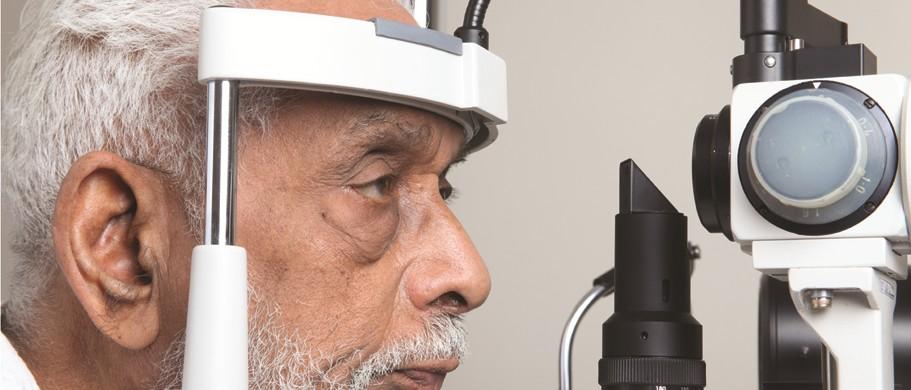
What is glaucoma?
Glaucoma is an eye disease caused due to increased pressure within the eyeball. It is also known as a “sneak robber of sightâ€Â, because if it is left unattended to, the pressure damages the optic nerve, leading to progressive, irreversible loss of vision.
Which are the two types of glaucoma?
Closed angle glaucoma: It often appears suddenly and is painful. Visual loss can progress quickly but the discomfort often leads patients to seek medical attention.
Open angle or chronic glaucoma: It tends to progress at a slower rate and the patient may not notice that they have lost vision until the disease has progressed significantly.
Once you have been diagnosed with glaucoma, the goal is to stop the progression of vision loss. For details on the treatments for glaucoma refer to the Treatments section.
What is retinal detachment?
Retinal detachment is a disorder in which the retina separates from its underlying layer of support tissue. The retina is a thin layer of light-sensitive tissue that translates images into neural impulses for the brain to interpret. Initial separation may be localised, but if left untreated, the entire retina may detach, leading to vision loss and blindness.
What are the causes of retinal detachment?
- Weak spots in the retina (lattice degeneration)
- Injury
- Long-term diabetes mellitus
- Myopia
- Retinal hole or tear
Sometimes retinal detachment occurs without any specific reasons.
To know more about the treatment options available for retinal detachment, refer to the Surgeries section.
What does eyelid and orbital disorder refer to?
These focus on abnormalities of the structures around the eye caused either due to injury to the eye muscle, congenital defects, nerve disorders or aging.
What are the kinds of eyelid and orbital disorders?
Ptosis: Ptosis is a condition whereby the natural position of the upper eyelid is droopy or sagging and limits a person's field of vision.
Entropion: Entropion is a medical term used to describe the sagging and inward turning of the lower eyelid and eyelashes.
Ectropion: Ectropion is a condition used to describe sagging and outward turning of the lower eyelid and eyelashes.
For more information on the treatments for the above, refer to the Treatments section.
Which are the known vision disorders in children that we address?
Squint is a known disorder in children that we address.
What is squint and what are its causes?
Squint is a condition in which the eyes do not look in the same direction. The movement of each eye is controlled by 6 muscles that pull the eye in various directions. A squint develops when the eye muscles do not work in a balanced way and the eyes do not move together correctly. Most squints are contracted in the first 3 years of your life.
What are the symptoms of squint?
Eyes do not look straight ahead. It is quite normal in newborn babies because their eyes look cross occasionally, particularly if they are tired. When it is noticed in children beyond three months of age, it is advisable to go to an eye specialist.
When a child looks at a person with one eye closed, or with its head turned to one side, it may point to the fact that they are experiencing double vision and could be an indication that they have a squint in the eye.
What is Keratoconus?
Keratoconus is a slow and progressive weakening of the corneal tissue that leads to thinning of the cornea and its gradual outward bulging.
How do I know if I have Keratoconus?
Blurry and distorted vision, observing of multiple images, poor night vision and increased sensitivity to light are some of the common warning signs of Keratoconus. In its advanced stage, the disease can impair a patients ability to drive a car or read a print.
What are the causes of Keratoconus?
While the reasons for contracting it have not been deduced objectively, it is estimated Keratoconus can be caused due to genetic reasons, environmental factors and cellular abnormalities.
What is the treatment of Keratoconus?
A patient of keratoconus usually needs help in the form of spectacles (early cases), semisoft contact lenses (special forms like Rose K, scleral and piggy back lenses). In advanced cases however one needs corneal transplantation (DALK/PK). However in mild to moderate cases one can stabilize the condition with a procedure called Collagen Cross Linking.
Read more about Collagen Cross Linking in the Surgeries section.
What are the treatments available for refractive disorders?
Refractive disorders can be corrected by the use of either spectacles or contact lenses. Alternatively surgery is a long-term solution.
Refractive surgeries
Photorefractive Keratotomy (PRK): Candidates for PRK include patients who have a high number and thin cornea.
Phakic IOLs (Staar ICL): It is a process in which lenses are surgically implanted. People who wear thick glasses or contact lenses with high power and are not eligible for LASIK/PRK are recommended for Phakic IOLs.
LASIK: LASIK is one of the most commonly performed surgeries, used to correct vision in people who are nearsighted, farsighted, or have astigmatism.
For more details on LASIK refer to the Surgeries section.
What are the treatment options available for CVS?
Usually CVS can be avoided or minimised with the following precautions:
- Use anti-reflective coating on your computer screen
- Blink frequently
- Take frequent breaks while reading or working on the computer for a long time
- Ensure your computer screen is 6-8 inches below the eye level
- Maintain a distance of 20-30 inches between your seat and the screen
- Ensure your computer seating area is not right opposite to an AC vent as it can dry up your eyes
- Wear your eyeglasses even if you think you can do without them
With these precautions there are also eye drops that are prescribed depending upon the case. Visit an ophthalmologist if you face any kind of discomfort due to excessive work on the computer.
How can cataract be treated?
Unfortunately, cataract cannot be treated using eyeglasses or medications. Surgery is the only way to treat cataract.
Some of the most common surgical methods of treating cataract include:
Extra Capsular Cataract Extraction (ECCE): ECCE is a method of cataract surgery that involves removing the eye's natural lens while leaving behind the back of the capsule that holds the lens in place.
Small Incision Cataract Surgery (SICS): SICS is a technique that achieves the manual removal of a cataract by effecting an incision of about 6mm in the eye.
Phacoemulsification: Phacoemulsification is the removal of cataract through extremely small-sized incisions.
At Shree Eye Care, we offer phacoemulsification, as the only option to treat cataracts. Read further on Phacoemulsification in Surgeries section.
What are the commonly followed methods of treating dry eyes?
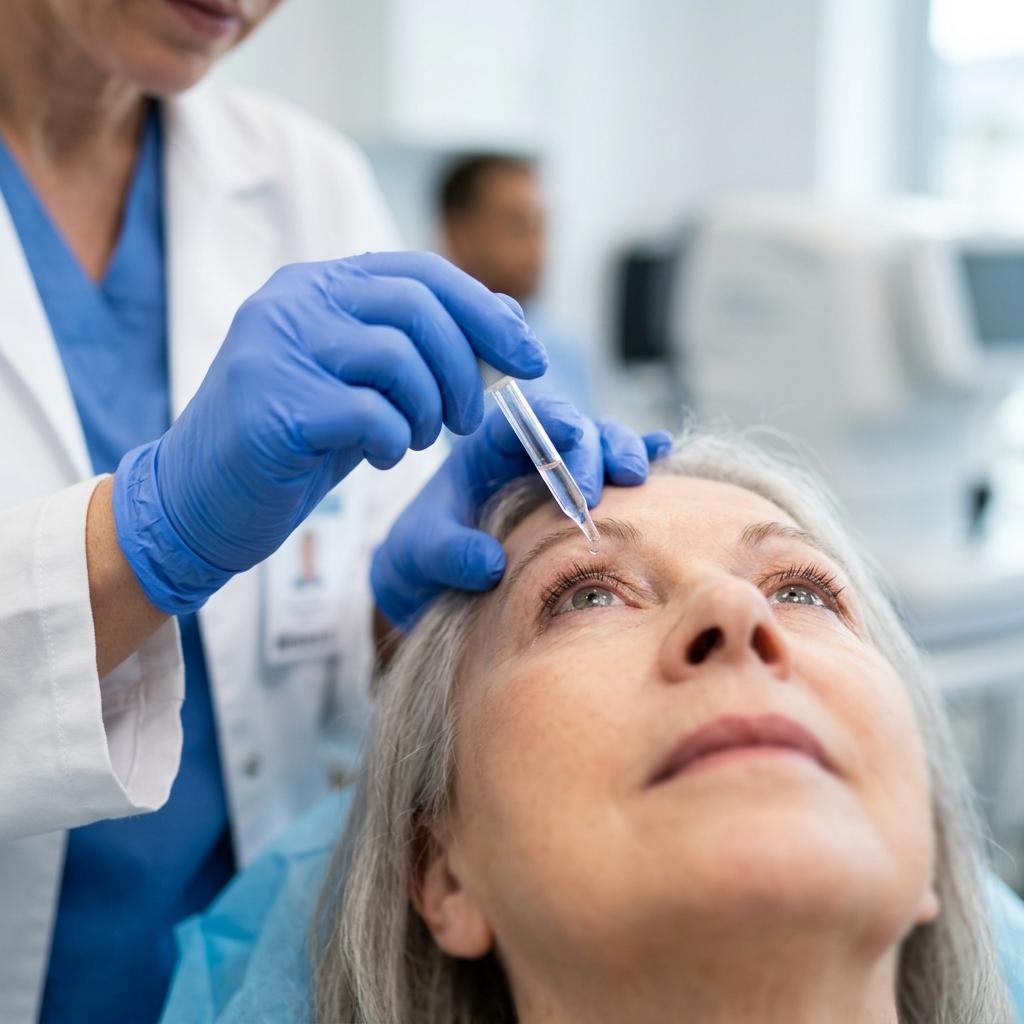
Artificial tear substitutes: Eye drops, also referred to as "artificial tears" are administered during the initial period. They lubricate the eyes and help maintain moisture.
Immuno-modulators and steroids: Your cornea specialist will decide if you need this advanced therapy.
Punctal occlusion: There is a channel that drains tears out of the eye into the back of your nose, and down your throat. Your cornea specialist may close this channel temporarily.
At Shree Eye Care, we are well-equipped to handle complex cases of dry eye syndrome.
What are the most common methods of treating glaucoma?
The most common methods of treating glaucoma intend to control the pressure in the eyes. There are three major methods of eye pressure control:
Drops: There are many effective medications that come to market every year that can make the drain function of the eye more efficient. This serves to lower the amount of fluid in the eye and decreases the pressure being placed on your optic nerve.
Laser: A laser may be fired directly into the drain of your eye with an intention of stimulating increased drainage.
Surgery: The main goal of surgery is to create a new drainage system for the eye.
To know more about the surgery, refer to the Surgeries section.
How can structural abnormalities of ptosis, entropion and ectropion be treated?
Ptosis, entropion and ectropion be treated through oculoplasty which is a specialised branch of ophthalmology, that focuses on abnormalities of the structures around the eye. It aims at improving function, comfort and appearance of structures around the eye including the lids and tear drainage system.
Ptosis or drooping eyelid often needs surgical correction which is best decided by your ophthalmologist.
Mild forms of ectropion and entropion can be treated with lubricating drops, ointments and eyeglasses. If these fail, the deformities have to be repaired surgically before the rubbing damages the cornea by causing infection and scarring.
At Shree Eye Care, all cases of oculoplasty are handled efficiently by our oculoplasty visiting consultant.
How is squint treated?
Treatment of squint comes under pediatric ophthalmology a subspecialty of ophthalmology concerned with eye diseases, visual development and vision care in children.
Diagnosis is an important step in handling squint patients. It should be diagnosed as early as possible. It is recommended that you go for routine checks to identify eye problems in babies and children. These checks are normally done in newborn babies and after 6-8 weeks of their birth. Routine preschool or school entry vision check can also be helpful in diagnosing squint.
Squint treatment helps preserve or restore vision and straighten the eyes. There are some treatment steps according to the type of squint.
Doctors recommend glasses that must be worn regularly to correct any refractive errors that maybe present.
Sometimes doctors prefer surgery to correct the appearance of the squint and also to restore binocular vision in some cases.
In many cases, an operation is recommended to make the eyes as straight as possible. Surgery is done to improve the appearance of the eyes.
In some cases, surgery may also improve or restore binocular vision. The exact operation depends on the type and severity of the squint.
At Shree Eye Care, all squint and pediatric cases are handled by our visiting pediatric ophthalmologist.
What is LASIK?
LASIK (laser-assisted in situ keratomileusis) is one of the most commonly performed surgeries done with the use of laser rays to correct vision in people who are nearsighted, farsighted or have astigmatism.
Who can undergo a LASIK?
Anybody above the age of 18 who wears spectacles or contact lenses can undergo this treatment. But it is not advisable for people whose number has changed significantly in the past year or is likely to change again in the future.
How is LASIK done?
An instrument called a microkeratome is used to cut a thin flap in the cornea. The cornea is then lifted back and the underlying corneal tissue is exposed to excimer laser rays to reshape. After the cornea is reshaped, the corneal flap is put back in place and the surgery is complete.
What are the advantages of LASIK?
- Very little pain
- Vision is corrected immediately or a day after LASIK is being performed
- Usually no bandages or stitches are required after LASIK
Is LASIK 100% safe?
With technology advancements, LASIK surgeries have become almost foolproof. However, it is always better to stay in sight of the following complications:
- The most possible complication of LASIK is eye infection, that may immediately follow the procedure. This infection can be controlled by the usage of antibiotic eye drops and other medicines
- Complications with the flap such as an incomplete flap, a free cap or an irregular flap are also possible. Normally, in such an event, the surgery is postponed and repeated after 3 months
- The third post-LASIK complication is an inflammation in the flap bed interface, leading to a reduction in vision. Sometimes, cells from the top surface of the flap (epithelium) migrate to the interface and grow there. Most of the times, lifting the flap and cleansing the interface can solve these problems. In rare cases, the flap may need to be cut away. In extremely rare cases, a corneal transplant may be necessary
- Another complication of LASIK is kerastecsia, or bulging of the cornea due to excessive thinning. This condition may lead to a severe drop in vision, and may be corrected by wearing hard contact lenses or through a corneal transplant
- Complications such as glares or halos around lights, especially at night, dry eyes, and an increased sensitivity to pain are also observed occasionally
What is the duration of surgery?
LASIK takes only about 10 minutes to complete per eye.
What are pre-operative processes to be followed for LASIK surgery?
Your ophthalmologist will do a detailed evaluation including a comprehensive eye checkup, a retinal evaluation, pachymetry (corneal thickness measurement) and topography (a map of the cornea) to find out if you are an eligible candidate for LASIK.
- If you are using soft contact lenses, you must revert back to using glasses for at least two weeks prior to the baseline evaluation. This will help restore the normal shape of the cornea
- If you are using semisoft (RGP) contact lenses, you must stop using them 3-4 weeks prior to the surgery
- You should avoid usage of creams, lotions or cosmetics on the face and eyes a day before the surgery
What care should be taken after undergoing LASIK surgery?
- When you shower, don't allow the water stream, soap or shampoo to hit your eyes. Do not allow dust particles or pet hair to get into your eyes
- Avoid going out in bright sunlight without sunglasses
- Don't let your eyes get too dry - use artificial tears as often as needed
- Don't rub your eyes while you're sleeping - a special mask, provided by your doctor will protect your eyes while sleeping
- It is absolutely imperative that you faithfully follow your doctor's schedule for medications, especially during the first week after your procedure
- Don't use the PC for more than one or two hours for the first week
- Avoid swimming, jacuzzis and saunas for the first month
Is there a chance of the refractive error coming back in the long run?
No. Once the healing process is complete, there are no chances of getting the number back.
What is phacoemulsification?
Phacoemulsification is the removal of cataract through extremely small-sized incisions.
What are the pre-operative precautions to be followed for phacoemulsification?
- Patients are usually required to remain fasting for 4 hours before the surgery
- Patients must disclose all medications to determine if they must be discontinued before surgery
- Blood-thinning medications may put patients at risk and they are discontinued, unless the risk for stroke is high
- You are required to undergo routine pre-operative investigation. Your personal physician (M.D.) needs to certify fitness for the surgery
- Your eye surgeon performs advanced testing to calculate your IOL (Intraocular Lenses) power
How is phacoemulsification done?
- The eye is made numb through the usage of anesthetic medications
- An incision or slit of approximately 2.5 mm is made in the eye, through which the tip of the instrument is introduced
- Localised high frequency waves are produced through this tip to rupture the cataract into very minute pieces, which are then sucked out through the same tip in a controlled manner
- A foldable lens is inserted through an incision or slit of approximately 2.5 mm made in the eye. In case of a non foldable lens implant, the incision must be enlarged to 5.0 or 5.5 mm
In most of the cases, no sutures are applied. However, your doctor may determine if you need a stitch for safety.
For best results, your eye surgeon may combine this with relaxing incisions (LRI's) to completely eliminate the need for glasses.
Intraocular Lenses:
At Shree Eye Care, we use a variety of intraocular lenses, according to the suitability of the patient.
Intraocular lenses are generally of two types, non foldable and foldable.
Among the foldable, the special types of lenses are:
Aspheric IOLs: These IOLs are designed for helping patients see very clearly, getting rid of vision abnormalities and ensuring better contrasts.
Toric IOLs: Foldable, single piece lenses that an eye surgeon implants during cataract surgery to replace the clouded lens. The unique design of these IOLs makes it possible to reduce or eliminate corneal astigmatism and significantly improve uncorrected distance vision.
Multifocal IOLs: These IOLs have been uniquely designed to provide enhanced image quality and a full range of vision – up close, far away and everything in-between – giving cataract patients the best opportunity to live life free of glasses.
What are the advantages of phacoemulsification?
- No stitches are required for 2.5 mm or smaller incisions. However for enlarged incisions (5.0 or 5.5 mm), one stitch might be required
- The technique uses smaller, self-sealing incisions that minimise the chances of any post-surgery complications
- Reduced healing time to help you resume work faster
- Less follow-ups
- Reduced chances of cornea distortion and astigmatism thus almost eliminating the need for glasses
- Recent advances and refinements in machine and microsurgical instruments have made it possible to carry out phacoemulsification using incisions that are less than 2.2 mm (MICS)
What care should be taken after phacoemulsification?
- Phacoemulsification allows for faster healing and the patient can get back to his/her normal routine as soon as possible
- The patient is advised to rest for at least 24 hours, until he or she returns to the surgeon's office for follow-up
- Only light meals are recommended immediately after the surgery
- Severe pain, nausea, or vomiting should be reported to the surgeon immediately
- Patients are advised to wear an eye shield while sleeping, and refrain from rubbing the eye for at least two weeks
- After the healing process, the patient will probably need new corrective lenses, at least for close vision
Shree Eye Care leverages the latest technological advancements in Phacoemulsification and offers different packages for the surgery according to the type of lens chosen. For further details contact us.
What is corneal transplantation?
Corneal transplantation is replacing a diseased front portion of the cornea with a healthy donor tissue. Traditionally, corneal transplants involve replacement of the full thickness of cornea (Penetrating Keratoplasty). However, with advanced research and technology, selective replacement of the diseased layer is possible. These are called lamellar transplants.
In case I am diagnosed with corneal disorders, can I go for a corneal transplantation immediately?
Once your corneal surgeon checks your eye for any corneal disorders and confirms the need for a transplant, you need to first get in touch with an eye bank, which registers your case.
As soon as a fresh cornea is available for grafting, the eye bank will inform you about the same. Your corneal surgeon will then help you get ready for the transplantation process.
What are the pre-operative routines to be followed for corneal transplantations?
- If you experience fever or infection in any part of your body within 2-3 weeks of your scheduled date of surgery, you can ask for the surgery to be rescheduled
- Any active eye infection or eye inflammation usually needs to be brought under control before surgery
- Blood-thinning medications may put patients at risk and they are discontinued, unless the risk for stroke is high
What are the different types of corneal transplants available?
Process:
- A button shaped piece of your damaged cornea is removed
- A button of the clear donor cornea is cut & placed on the eye
- The new cornea is stitched onto your own cornea using nearly invisible sutures
Duration of surgery: About an hour.
Advantages: Good optical clarity.
Process:
- The cornea is dissected to almost 95% thickness and the top layer is removed
- A donor corneal button is prepared by removing the two inner most layers of the cornea viz. Descemet's membrane and donor endothelium
- The donor graft is then sutured to the host
Duration of surgery: About an hour.
Advantages:
- Closed eye surgery
- Better chances of success
Process:
- The inner two layers of the diseased cornea are peeled off
- A donor cornea is then split or dissected to create a flap of the inner two layers and a third layer of stroma
- This 3 layer donor is then folded and inserted into the eye and floated up to stick onto the inside of the cornea replacing the layers removed earlier
Duration of surgery: Less than an hour.
Advantages:
- Closed eye surgery
- Gets completed quickly
- Faster visual recovery
What care should be taken post corneal transplantation?
- An eye shield or glasses must be worn until the surgical wound has healed
- Eye drops will be prescribed for the patient to use for several weeks after the surgery to prevent infection and reduce inflammation. Some patients require medication for at least a year
- For the first few days after surgery, the eye may feel scratchy. Blurred vision may persist for several months
- Sutures are often left in place for 6 months, or for as long as 2 years
- Rigid contact lenses to reduce corneal astigmatism that follows corneal transplant may also be prescribed
At Shree Eye Care, Dr. Priya Srinivas handles referral cases of corneal diseases needing opinion and surgery, referred by general ophthalmologists and has 5 years of experience in treating complex corneal disorders.
How is the surgery for glaucoma done?
The main goal of surgery is to create a new drainage system for the eye. This can be done by fashioning a trap door on the surface of the eye to allow pressure and fluid build-up to escape when there is an excess within the eye.
How can the damage caused by glaucoma be determined?
First, a determination is made as to how much damage your optic nerve has sustained and how much of your corresponding vision has been lost.
A direct visualisation of your optic nerve is made and an estimate of the amount of damage can be inferred.
The amount of vision loss is judged with a visual field test (perimetry). Once the test is over, a diagram of your vision with many measurements is printed out and followed over time. If progression on this vision assessment test can be documented, you may need a more intensive treatment.
What care should be taken after the surgery?
- Wear an eye shield for at least 2 days after the surgery
- Avoid lifting heavy objects and keep your eyes away from water
- If your eye swells or if there is a fluid formation, visit your doctor
- Carry an umbrella or wear shades when travelling in the hot sun
- Keep your eyes away from water as it can be disastrous
For any further details on glaucoma, visit Shree Eye Care.
What are the treatment procedures for retinal detachment?
Pneumatic retinopexy: The retinal detachment is repaired by injecting a gas bubble into the eye after which laser or freezing treatment is applied to the retinal hole. The patient's head is then positioned so that the bubble rests against the retinal hole.
Scleral buckling: Scleral buckle surgery is an established treatment in which the eye surgeon sews one or more silicone bands to the white outer coat of the eyeball. The bands push the wall of the eye inward, and reattaches the retina back to the support tissue.
Vitrectomy: Vitrectomy involves the removal of the vitreous gel, post which the eye is filled with a gas bubble or silicon oil.
Laser photocoagulation: Used in conjunction with vitrectomy or scleral buckling. In laser photocoagulation, the surgeon directs a high-energy laser to burn small pinpoints on the retina. For a retinal tear or hole, the burns create scar tissue, which attaches the retina to the underlying tissue.
What care should be taken after the surgery?
- The first week after your surgery, take it easy; walk and move your head in slow motion
- In case of pneumatic retinopexy, patients may have to keep their heads tilted for several days to keep the gas bubble in contact with the retinal hole. Also, it is advised to avoid flying until the gas bubble is gone
- You may shower and wash your hair carefully. Do not scrub your head vigorously. Avoid getting soap and water in your eye
- You may use over-the-counter non-aspirin analgesics and warm compresses, to relieve any minor discomfort
- Use prescription pain medications as instructed by your physician. If you experience severe pain, please inform your doctor
All retinal cases at Shree Eye Care are handled by our visiting retinal subspecialist.
What is collagen cross-linking?
Collagen cross-linking is a procedure used to slow down the advance of Keratoconus (abnormal protrusion of the cornea).
How is collagen cross-linking performed?
A one-time application of riboflavin and a photosensitizing agent is administered to the eye after removing the skin from the surface of the cornea. The eye is then exposed to UV-A light for approximately 30 minutes.
How does collagen cross-linking help lessen the effect of keratoconus?
Collagen cross-linking helps recover and preserve the mechanical strength of the keratoconus-affected cornea. The process increases the corneal rigidity significantly and arrests any further progress of keratoconus. Owing to this, any further degeneration of the cornea can be checked and the need for corneal transplantation can be avoided.
What are the post-operative imperatives to be followed for collagen cross-linking?
Your cornea specialist will place a bandage contact lens over the treated eye. You will be asked to apply antibiotic and steroid drops for a while. The vision will be blurry for a while before returning to normal. Also, it may necessitate the refitting of a contact lens or a change in the spectacle number.

Meeting challenges and ensuring reliability
Case Study 1 6 August, 2010
A 60 year old lady residing in rural Maharashtra was brought for the surgery of a very challenging condition known as double headed pterygium. The surgery was confidently and successfully completed using an advanced technique (conj autograft with tissue glue, sutureless).
The patient’s vision returned to normal.
Case Study 2 23 June, 2010
A 70 year old diabetic lady was referred by a fellow doctor for an opinion regarding corneal problem. On examination and case study, it was found that patient’s cornea was melting and suggested an urgent treatment with a glue (cyanoacrycate). The treatment resolved the corneal problem and the patient recovered fully.
Case Study 3 17 May, 2010
A 62 year old, diabetic female was referred to Shree Eye Care for an infection of the cornea which she developed after 1 month of her cataract surgery.
With expertise in corneal diseases, she was investigated accordingly and treated with an emergency corneal transplant. Her vision improved dramatically and she was found to also have some infection in the vitreous cavity (back portions of the eye). She was under the care of a cornea specialist and also a retina specialist. She is on the road to recovery now.
Case Study 4 29 April, 2010
A 63 year old gentleman was referred to us for a fleshy growth in the left eye which was treated with antibiotics and medication.
On examination, he was found to have a cancerous growth. He was advised an excision of the growth. The same was done (excision + double freeze thaw cryotherapy + amniotic membrane) and the tissue was sent for a biopsy.
At the end of 3 months, he was comfortable and had no recurrence.
Case Study 5 12 April, 2010
A 23 year old medical student was referred to us by another ophthalmologist for a suspected corneal infection and white spot in the cornea after some dirt entered into her eye.
After a scraping of the corneal tissue and sending for microbiological evaluation, she was advised to use antibiotic eye drops.
Within a week, she resolved completely and regained her eyesight.
Case Study 6 7 April, 2010
A 50 year old man was referred to us for an eye infection which was not responding to medications. On careful examinations, he was diagnosed to have a corneal ulcer which was treated with antibiotics. But it was also noted that the posterior segment of the eye, the vitreous had got infected. He was managed by the expertise of our vitreo retinal surgeon by giving intravitreal injections of antibiotics. Gradually his infection was totally cured.
This emphasises the importance of having expert superspeciality (cornea + retina) care at hand.
Case Study 7 1 April, 2010
A 44 year old woman was referred for a cornea opinion by another specialist. She was suffering from hazy vision in her left eye. She was diagnosed to have corneal infection by a virus. After appropriate treatment, her vision completely improved to normalcy and her cornea was cleared.
Case Study 8 28 December, 2009
A 30 year old male was referred to us for redness which was persistent for a month in the left eye which was not responding to medications. On careful examination there was a foreign body with surrounding corneal infection in the left eye - cornea.
Removal of the foreign body and treating with appropriate medications led to gradual and complete resolution of the problem.
